Angelman Syndrome (AS) is a rare neurogenetic disorder that affects approximately one in 15,000 people – about 500,000 individuals worldwide. Children and adults with Angelman syndrome typically have balance issues, motor impairment and debilitating seizures. Some individuals never walk. Most do not speak. Disrupted sleep cycles also can be a serious challenge to the individual and caretakers. Individuals with Angelman syndrome require continuous care and are unable to live independently, and they have a normal life expectancy.
Foundation for Angelman Syndrome Therapeutics (FAST) is the charity organisation that was founded in 2008 in the USA with a mission to cure Angelman syndrome. Today, with operations also in Australia, Canada, France, Italy, Poland, Spain and here in the UK, FAST has become the largest non-governmental funder of AS research.
Traits and Symptoms of Angelman Syndrome
Many of the typical characteristics of Angleman syndrome (AS) are not evident at birth. However, some individuals with AS may have nursing and feeding difficulties starting in infancy. More noticeable delays in development are usually evident around 6-12 months of age. It is important to note that Angelman syndrome is a spectrum disorder, so not all individuals exhibit the same behavioral characteristics or preferences.
Most common traits:
- Normal prenatal and birth history, normal head circumference at birth, no major birth defects.
- Normal metabolic, hematologic, and chemical laboratory profiles.
- Structurally normal brain by magnetic resonance imaging (MRI) or computed tomography, although mild cortical atrophy or dysmyelination may be observed.
- Delayed attainment of developmental milestones without loss of skills.
- Evidence of developmental delay by age 6 to 12 months, eventually classified as severe.
- Speech impairment, with minimal to no use of words; receptive language skills and nonverbal communication skills higher than expressive language skills.
- Movement or balance disorder, usually ataxia of gait and/or tremulous movement of the limbs.
- Behavioural uniqueness, including any combination of frequent laughter/smiling; apparent happy demeanor; excitability, often with hand-flapping movements; hypermotoric behavior; short attention span.
Additional traits:
- Delayed or disproportionately slow growth in head circumference
- Abnormal electroencephalogram (EEG), with a characteristic pattern of large-amplitude slow-spike waves.
- Seizures, usually starting before age 3
- Suck/swallowing disorders
- Muscle hypotonia during infancy
- Excessive chewing/mouthing behaviors, including non-edible objects
- Strabismus
- Hypopigmented skin, light hair and eye color (compared with family); seen only in those with a deletion.
- Hyperactive lower-extremity deep-tendon reflexes
- Wide-based gait with out-going ankles
- Abnormal sleep-wake cycles and disrupted sleep
- Attraction to/fascination with water
- Scoliosis
- Constipation
Genetics and types of Angelman Syndrome
Angelman Syndrome is a single-gene disorder caused by a loss of function in the UBE3A gene on the maternal 15th chromosome. People have two sets of chromosomes – one inherited from the mother and one from the father. Each chromosome contains hundreds to thousands of genes, where a gene is a single unit of genetic material (DNA) that acts as an instruction for the way an individual is made and develops.
In a typical person, the maternally inherited UBE3A gene is active, while the copy of the gene inherited from the father is “silenced” in the neurons in our brains – a phenomenon known as imprinting. For people with Angelman syndrome, this maternal gene isn’t able to be properly read, which impacts it’s messenger RNA (mRNA).
Consider mRNA as the cellular interpreter of DNA’s instructions, transforming them into a language the cell can understand. In individuals with Angelman syndrome, a malfunction in the UBE3A gene disrupts this intricate communication process between the DNA and the cell’s protein synthesis sites. Consequently, the neurons fail to produce a working version of the UBE3A protein, resulting in the symptoms of Angelman syndrome.
In most cases, Angelman syndrome isn’t inherited. There are 6 recognised types of the syndrome:
Deletion
- A deletion is caused by a missing piece of DNA in region 15q11-13 on the maternal chromosome 15.
- 65–75% of all cases
Mutation
- Occurs when there is a small abnormality in the DNA of the UBE3A gene. A mutation can happen anywhere on the gene.
- 5-11% of all cases
Paternal uniparental disomy (UPD)
- An individual with UPD has two copies of chromosome 15 from their father, both of which are silent, instead of one each from the father and mother.
- 3–7% of all cases
Imprinting defect (ICD)
- Occurs when the mother’s chromosome 15 is blank, and the imprinting centre (a small stretch of DNA in the q11-13 region) copies the father’s chromosome 15.
- <3% of all cases
Mosaic
- This is an extremely rare genotype of Angelman syndrome where a small proportion of the body’s cells are expressing UBE3A. A person with mosaicism has a mixture of fully expressing and non-expressing UBE3A DNA in the cells of the body.
- 1% of all cases
Other
- In addition, there are also people whose testing for Angelman syndrome is normal, but who still meet the diagnostic criteria for AS. These individuals may have as yet unrecognised mutations that affect UBE3A or genomic imprinting on Chromosome 15.
- <10% of all cases
Angelman testing and Diagnosis
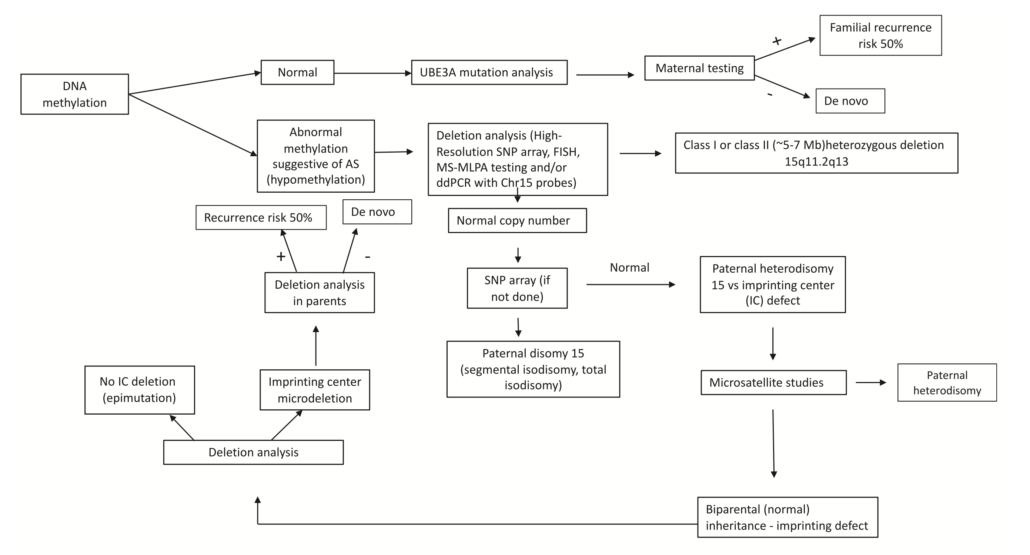
The Methylation test may also be called Southern Hybridization Methylation Specific PCR Assay or Methylation Specific PCR Test. The key word is “Methylation” and it is the most sensitive diagnostic test for Angelman syndrome. This test will positively identify about 80% of individuals with Angelman syndrome. Methylation refers to a chemical “tag” added to DNA and can be used to identify whether the DNA was contributed by the mother or the father. Where this tag is added occurs in a distinct pattern if it came from the mother and a different distinct pattern if it came from the father. The pattern of this tag can be examined to determine which parent contributed the DNA. The DNA methylation test will determine if an individual has one of each pattern (one from each parent) or an Angelman syndrome pattern (where only the pattern from the father is present.)
If an individual has a positive methylation test for AS and a positive FISH test for loss of Chromosome 15, then we know the person has Angelman syndrome caused by a deletion. This is the most common cause of AS and about 70% of individuals with AS have this deletion. These deletions can occur randomly months before the mother was even born. A woman’s eggs form when she herself is a fetus at about five months gestation. The chromosomes in her developing eggs are rapidly duplicating and separating as the eggs multiply, and errors in chromosome structure can easily occur at this stage. These cell errors are common and usually harmless. Most eggs containing errors, if fertilized, fail to develop and do not result in pregnancy. Some deletions are harmless and can result in a perfectly typical baby. Deletions are a problem in the small number of cases where the paternal chromosome that will later fertilize the egg cannot compensate for the missing information. This is what occurs in Angelman syndrome. Chromosome deletions are relatively common and there is no evidence that anything specific caused it or could have prevented it; it is simply random.
Trials and searching for cure
Scientists believe that Angelman Syndrome has the greatest potential for being cured when compared to other neurogenetic disorders, and FAST has a plan well underway to achieve just that.
Learn how to help by donating, fundraising or participating in studies here.